ABOUT BREAST CANCER

Did you know that breast cancer can affect all genders, includinG men, whether assigned at birth or not?
It’s important to raise awareness for everyone facing a CANCER diagnosis, regardless of their gender identity.
Awareness and compassion save lives

Learn to check your breasts!
Breast checking is about knowing what feels normal for you. There’s no single “right” way your breasts should look or feel. The key is noticing changes.
Most breast changes are not cancer, but spotting something unusual early can make a real difference. Checking regularly helps you feel confident about your own body and means you’re more likely to notice if something isn’t right.
You don’t need special equipment. Just take a few minutes regularly to look and feel in a way that suits you. If you notice unusual changes, contact your GP.
This guide will walk you through it step by step.

What’s New in Breast Cancer Care
Research in breast cancer therapy is moving quickly, with new approaches offering better options for those with early stages and advanced disease.
Scientists are developing treatments that are more targeted, more precise, with fewer side effects and able to work even when cancers become resistant to standard care.
There’s also growing progress in immune-based therapies and personalised medicine, helping doctors tailor treatment to each patient. Together, these advances are creating more hopeful paths forward and improving both outcomes, therapies impact and quality of life.

Alcohol and Breast Cancer Risk Explained
Alcohol is classified as a carcinogen and is linked to several cancers, including breast cancer.
Research shows that even low or moderate drinking raises breast cancer risk. The more you drink, the higher the risk. Wine, beer and spirits all contain ethanol.
No type of alcohol is safer when it comes to cancer risk. It can increase oestrogen levels and damage DNA, both of which are linked to breast cancer development.
Less is better. Reducing, avoiding or choosing alcohol-free options can help lower breast cancer risk over time. This is one of the few breast cancer risk factors you can actively change.

Breast Cancer Day by Day: Simple Habits That Make a Tough Journey Easier
A grounded, day to day guide for navigating breast cancer with a bit more ease. It covers some simple routines that make treatment days smoother, practical habits for managing side effects, ways to stay healthy and to protect your emotional wellbeing when things feel overwhelming.
It also highlights practical tools for staying organised, knowing what to ask your medical team and building a support system that actually helps.
Clear, calm and realistic advice to help you feel steadier and more in control throughout the journey.

the Most Studied Risk Factors for Breast Cancer
Breast cancer risk comes from a mix of age, genetics, hormones, lifestyle and personal health history.
Some risks can’t be changed, but others can be reduced with practical steps such as staying active, limiting alcohol and maintaining a balanced weight.
Understanding these factors helps people make informed choices, keep up with screening and feel more confident about their long term health.

Breast Cancer Awareness for Younger Women
Breast cancer in younger women is less common, but it does happen. Awareness at a younger age helps people notice symptoms sooner and feel confident seeking help, rather than brushing things off as stress or hormonal changes.
It’s important to offer clear information and accessible training so younger women know what to look for and when to act.
Understanding the signs, trusting their instincts and recognising changes early can make a real difference to outcomes and peace of mind

Breast Awareness: Why Knowing Your Normal Matters
Being breast aware isn’t about constant checking or worrying. It’s simply about getting to know what’s normal for your body so you can spot changes early.
Most breast changes aren’t cancer, but recognising something unusual and speaking to a clinician promptly can make a real difference. Acting quickly can save lives.
It is essential to learn what to look for, when to act and when to advocate for yourself. Awareness is one of the most effective tools we have for early detection.
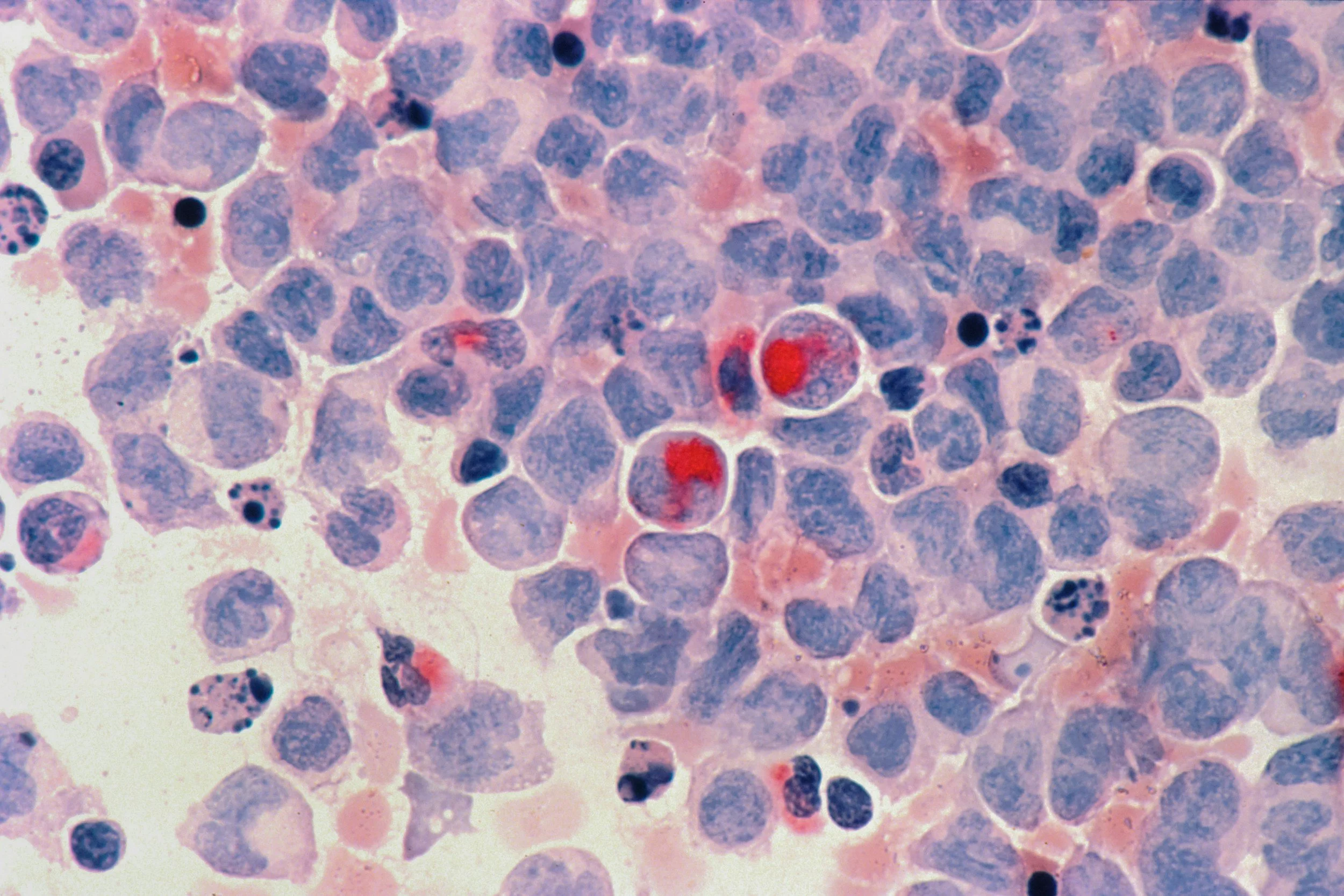
Understanding Breast Cancer Recurrence: What Research Tells Us
Understanding breast cancer recurrence can feel worrying, but having clear information helps make it less overwhelming.
Recurrence simply means that cancer returns after treatment, and it can happen in different ways: in the breast area, nearby lymph nodes or elsewhere in the body.
Researchers have identified several medical factors that can influence risk, such as tumour type, lymph node involvement and hormone receptor status.

Why Early Detection Still Saves Lives
Despite huge advances in treatment, early detection remains one of the strongest factors in improving outcomes for any type of breast cancer.
When changes are found early, treatment options are often more effective and less intensive. Yet many people delay seeing a doctor because they’re unsure what symptoms matter, feel embarrassed, or worry about wasting someone’s time.
The aim is to encourage confidence, reduce hesitation and help people feel empowered to take action when something doesn’t feel right. If you’re concerned, it’s always reasonable to ask for a proper check up and ensure your concerns are properly addressed.

Breast Cancer Myths That Hold Us Back
Misconceptions about breast cancer are still common and can stop people seeking help when they need it.
From the idea that only older women are at risk, to beliefs about pain, bras and lifestyle triggers, these myths create confusion and unnecessary worry.
It’s important to clear up some of the most persistent misunderstandings and offer simple, evidence-based information so people feel better informed and less misled. Clear guidance helps reduce fear, encourages timely check-ups and makes it easier for everyone to recognise what genuinely matters and what doesn’t.

Breast Cancer and Exercise: Why Moving More Matters
Research shows that being physically active is one of the strongest modifiable ways to lower the risk of several cancers, including breast cancer.
Regular exercise isn’t just good for your heart and mood, it also influences hormones, inflammation and body weight in ways that help reduce cancer risk.
Guidelines recommend at least 150 minutes of moderate activity or 75 minutes of vigorous activity per week, plus muscle-strengthening exercises at least twice a week. More activity continues to add benefit, and even light activity such as daily walking can reduce overall cancer risk

Complementary Therapies in Cancer Care: What the Evidence Says
When facing a cancer diagnosis, many people look for ways to feel better and cope alongside conventional treatment. Some non-medical practices can help with symptoms, side effects and quality of life when used in addition to, not instead of, medical care. It’s important to talk to your treatment team before trying anything new.
Complementary therapies like meditation, yoga, acupuncture and massage can help with emotional wellbeing, reduce specific symptoms and improve quality of life during cancer treatment.
There are some evidence-based addition to complementary therapies such as Chinese medicine, relaxation frequencies, and supplements after treatment, all grounded in scientific data and reputable research.

GROWING LINK BETWEEN NUTRITION AND BREAST CANCER
Recent research is increasingly showing how diet and nutrition can influence both breast cancer risk and recovery.
According to the British Nutrition Foundation, a balanced diet with plenty of fibre, vegetables and whole grains can help manage hormone levels and inflammation, which may support better outcomes.
New studies also suggest that optimising your eating patterns during treatment may make standard therapies more effective and better tolerated.

Why joy matters during breast cancer treatment
When we talk about breast cancer, the focus is often on treatment, side effects and survival rates. These conversations are essential, but they can leave little space for something equally important: joy.
Joy may seem secondary during treatment. In reality, it plays a meaningful role in how people cope, connect and move through the experience.
Moments of joy are not about ignoring reality. They are about creating space within it. This is one of the reasons spaces outside hospitals matter. They allow people to be seen not just as patients, but as individuals with identity, personality and life beyond the diagnosis.

Life after diagnosis: redefining identity
A breast cancer diagnosis does not only affect the body. It can also change how a person sees themselves.
For many, identity becomes something to navigate as much as treatment itself.
Hair, energy levels, routines and even the way others respond can change quickly. These shifts can affect confidence, self-image and the sense of who you are.
It is common to feel disconnected from your body or from the version of yourself you once recognised. These feelings are not superficial. They are part of a deeper process of adjustment.

